Diagnostic Mammogram
Diagnostic mammograms are specialized mammograms designed to solve a particular problem. The radiologist designs each exam in order to answer the particular question at hand.
Reasons to have a diagnostic mammogram:
- Question arising from a screening mammogram
- Breast symptom such as a lump, focal breast pain or nipple discharge
- Follow-up exams
- Personal history of breast cancer
In addition to the four views obtained in a screening mammogram, there are many specialized views that are possible to further investigate a finding. The most common view is called a “spot compression magnification” view. This is a magnified view of a particular area of the breast. The radiologist may also want to do an ultrasound.
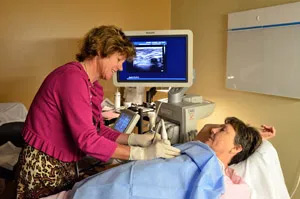
Breast Ultrasound
Ultrasound uses sound waves to generate a picture of the breast tissue. No compression is necessary. Ultrasound is particularly useful in telling cysts from solid masses in the breast. Cysts are very common and totally benign; about half of all women have some cysts in their breasts at some point. Ultrasound is also very helpful in characterizing masses and lumps.
Sometimes we do find a lesion that requires a biopsy to find out what it is. Fortunately, the vast majority of breast biopsies can be accurately performed with a needle and do not require surgery. Depending on the finding, a needle biopsy is performed, using either stereotactic (mammogram), ultrasound, or MRI guidance.
Breast Biopsy
Stereotactic-Guided Breast Biopsy. The stereotactic table is specially designed so that you can lie face-down with one breast positioned through a hole in the table. Two digital x-ray images are taken from different angles, allowing the radiologist to precisely localize the area to biopsied. Once the area has been located, the radiologist numbs the area with a local anesthetic, then uses computer guidance for precise needle placement and collection of small tissue samples.
Ultrasound-Guided Breast Biopsy. The radiologist uses ultrasound to locate the area for biopsy and to direct the needle used in collecting breast tissue samples.
Both methods are as accurate as a surgical biopsy and are performed on an outpatient basis, taking less than 40 minutes to perform and requiring no stitches. Furthermore, the patient can resume normal, non-strenuous activities immediately after the procedure is done. The samples are sent to the pathology lab for analysis. Results are usually available within 48 hours.
MRI-Guided Breast Biopsy. We can perform a standard needle biopsy in the MRI suite if a lesion is detected only on a Breast MRI exam, and this can be performed in under an hour.
Magnetic Resonance Imaging of the Breast
MRI is a technique using a very strong magnet and radio waves to pick up signals from the breast tissue. We use state-of-the-art equipment including a dedicated bilateral breast surface coil. The patient lies face-down within the scanning field for approximately 25 minutes. The primary way that abnormal tissue stands out on MRI is because it gets more blood flow than the remaining tissue. We can detect blood flow by taking images before and after infusion of an intravenous substance (gadolinium) that is easily seen on MRI. Breast MRI is most useful in detecting breast cancer and evaluating the integrity of implants. Breast MRI is often employed in patients with a known breast cancer in whom there is a question about how extensive the disease is. Medical indications (reasons) for breast MRI are evolving, and are the subject of many studies around the country.
We utilize a special computer-assisted detection (CAD) program designed for the processing and interpretation of Breast MR Images.
Ductography
A ductogram, also called a galactogram, is a test done if you are having persistent nipple discharge from a single duct, and your mammogram is normal. A tiny tube is inserted into the duct and a tiny amount of iodine contrast dye is injected into the duct. Several mammogram pictures are then obtained, with the ducts outlined by the iodine contrast dye. This shows whether there is anything inside the duct which could be producing the discharge. Most women report that this is not painful. When the duct is filled with fluid, it may feel a cramping sensation similar to what many women experience with their menstrual cycle.
